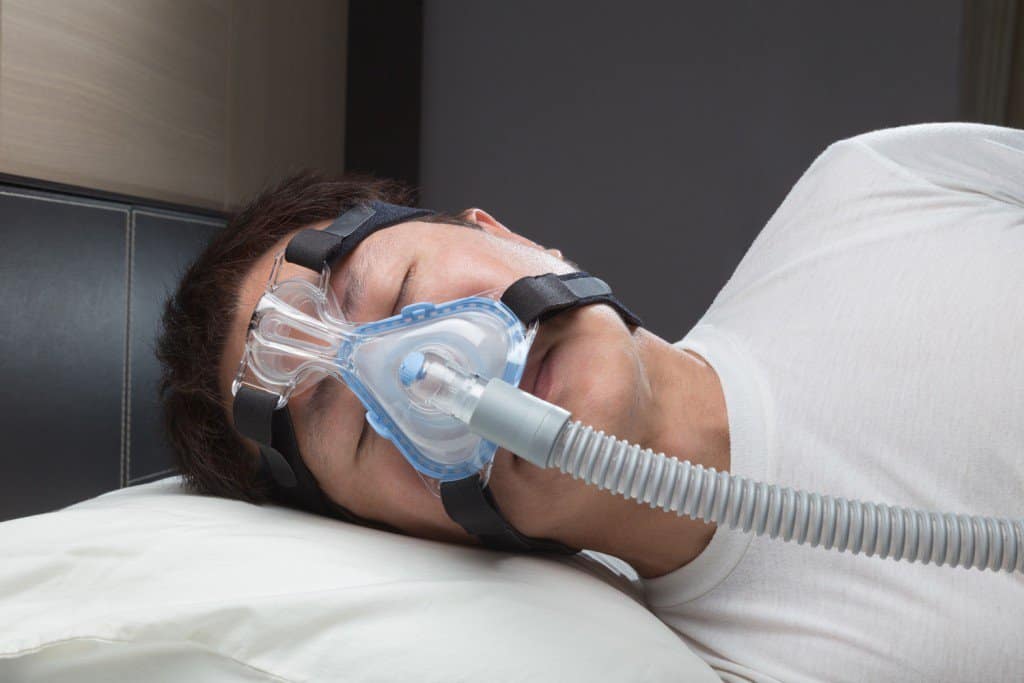
Obstructive sleep apnea (OSA) is a chronic sleep disorder that affects about 30 million people in the United States. (1) Worldwide, it’s estimated that 425 million people struggle with the condition. (2) Currently, the premier diagnostic tool for OSA is the apnea-hypopnea index (AHI) — but it looks like researchers out of Mount Sinai are about to shake things up. (3)
More specifically, the Mount Sinai Sleep and Circadian Analysis (SCAN) Group developed a new automated metric they coined “ventilatory burden.” (4) The group, led by Ankit Parekh, Ph.D., says the automated breath-by-breath measure can not only determine the severity of a patient’s obstructive sleep apnea and their risk of mortality as a result of the condition, but it can also predict both short and long-term consequences of the disorder like coronary heart disease — all based on a routine sleep study.
Where We Are in Diagnosing OSA
Obstructive sleep apnea is a common sleep disorder characterized by the partial (hypopnea) or total (apnea) collapse of the airway during sleep. (5) And the science behind it is easy enough — during sleep, the muscles at the back of the throat relax enough to impede breathing. (3) Apneas can be as short as 10 seconds or as long as 20 seconds. The number of apneic episodes per night varies from person to person, but it’s not uncommon for those with severe sleep apnea to have hundreds of events per night. Common symptoms of OSA include loud snoring, gasping for air during sleep, fragmented sleep, and excessive daytime sleepiness. (3)
The apnea/hypopnea index (AHI), which measures the average number of apnea or hypopnea events in one hour, is the go-to diagnostic tool for OSA. Doctors typically use the AHI to categorize a patient’s sleep apnea as mild, moderate, or severe. (3)
- Mild sleep apnea: The sleeper has 5 to 15 apnea or hypopnea events per hour
- Moderate sleep apnea: The sleeper has 15 to 30 events per hour
- Severe sleep apnea: The sleeper experiences more than 30 events per hour
While measuring AHI’s is currently the best tool we have for diagnosing OSA, the team at Mount Sinai Sleep and Circadian Analysis (SCAN) Group points out that the metric has its limitations. “The AHI is a simple and ineffective metric when it comes to analyzing sleep apnea severity,” says Parekh. “The cutoffs and rules that are used to calculate AHI are subjective and therefore highly variable.” In addition to variables like the subjectivity of the scorer, Parekh adds that the “AHI can also influenced by several other factors, including noise, device type, and time spent sleeping. etc.”
According to Parekh, “The ventilatory burden, the way we have defined it, cleanly represents an individual’s expression of upper airway obstruction on a routine sleep study — free of any sources of noise. It is not based on any subjective rules and does not differ based on device type, etc.”
A New Diagnostic Tool For Obstructive Sleep Apnea?
Using data from two community cohorts, including the Brain Aging and Sleep Center at NYU Langone Health and the Federal University of São Paulo in São Paulo, Brazil, Parekh and his team established a baseline for the normative range of ventilatory burden by analyzing more than 34 million breaths from over 5,000 participants. They then assessed
- The relationship between the degree of upper-airway obstruction and ventilatory burden
- The relationship between ventilatory burden and mortality risks, including cardiovascular disease (derived using an automated algorithm)
- The relationship between ventilatory burden and hypertension and sleepiness
Ultimately, the team found that not only did the automated measure of ventilatory burden prove to assess the severity of obstructive sleep apnea effectively, but it also sidestepped the pitfalls typically associated with AHI, like instability from one night to the next, for example. Moreover, the new measure took things one step further by predicting patients’ mortality associated with cardiovascular diseases.
“In the field of sleep medicine, increasing attention is being placed on replacing the AHI with a better metric,” says Parekh. “However, so far, few, if any, metrics have been systematically investigated, including defining the normal vs. abnormal cutoffs and their variation from one night to another. With our recent study, using the cutoffs we have defined, we can prioritize individuals in whom treatment of sleep apnea will be beneficial in terms of their cardiovascular disease sleepiness, or hypertension.”
“Our hope is that physicians can use the ventilatory burden metric to determine the type of sleep apnea treatment best suited for the patient, says Parekh. “Once this metric is incorporated clinically across sleep labs, the benefit to patients will be getting an accurate description of their sleep apnea and the peace of mind from knowing that treatment will be beneficial to them.”
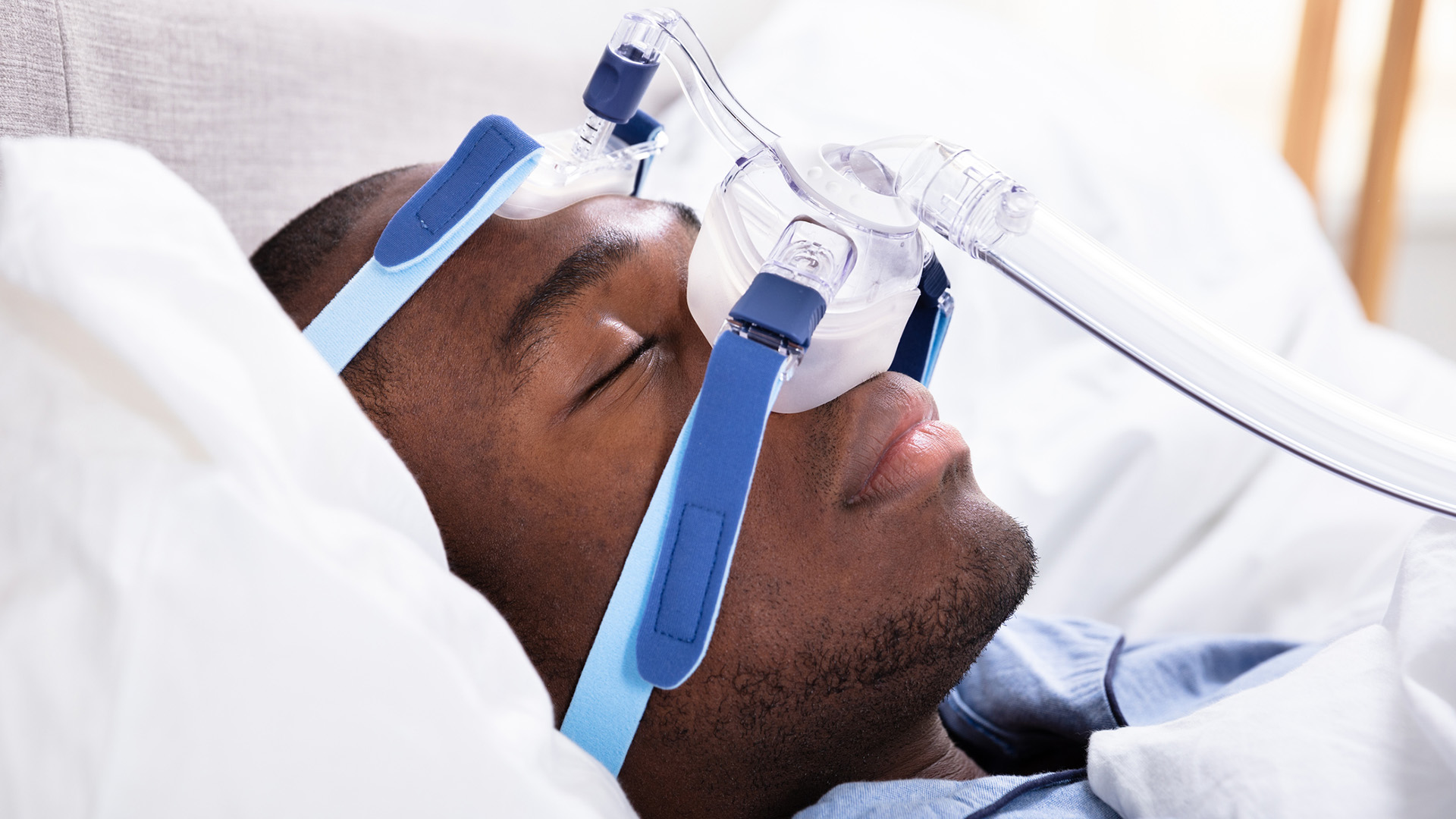
All May Not Be Equal in Sleep Apnea Research: New Data Shows Black Patients May Be Underrepresented
A Deep Dive Into Just How Badly the CPAP Machine Recalls Negatively Affected Doctors’ Mental Health
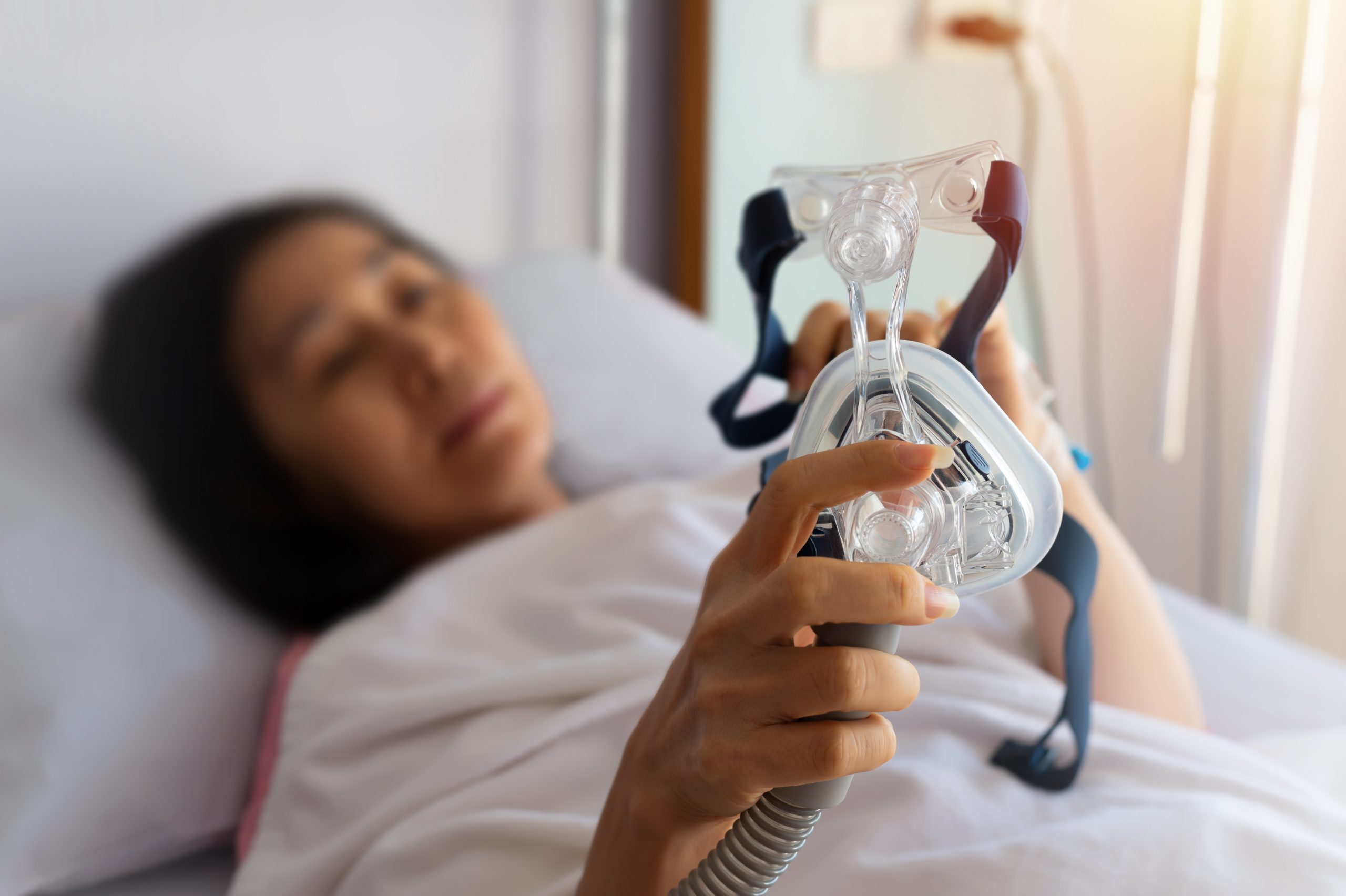
Early Clinical Trial Finds Epilepsy Drug Success for Sleep Apnea Patients
If We Want People to Use Their CPAP Machines, They Need to Be Easier to Use: Opinion
Sources
1. Goyal M, Johnson J. Obstructive Sleep Apnea Diagnosis and Management. Mo Med. 2017;114(2):120-124.
2. Benjafield AV, Ayas NT, Eastwood PR, et al. Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. Lancet Respir Med. 2019;7(8):687-698. doi:10.1016/S2213-2600(19)30198-5
3. Slowik JM, Sankari A, Collen JF. Obstructive Sleep Apnea. [Updated 2022 Dec 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459252/
4. Mount Sinai Health System (2023) Mount Sinai researchers develop novel, Automated Measure of sleep studies to determine severity of obstructive sleep apnea, Mount Sinai Health System. Available at: https://www.mountsinai.org/about/newsroom/2023/mount-sinai-researchers-develop-novel-automated-measure-of-sleep-studies-to-determine-severity-of-obstructive-sleep-apnea (Accessed: 26 September 2024).
5. Benjafield AV, Ayas NT, Eastwood PR, et al. Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. Lancet Respir Med. 2019;7(8):687-698. doi:10.1016/S2213-2600(19)30198-5
6. Parekh, Ankit. Author interview. September 25, 2024.
