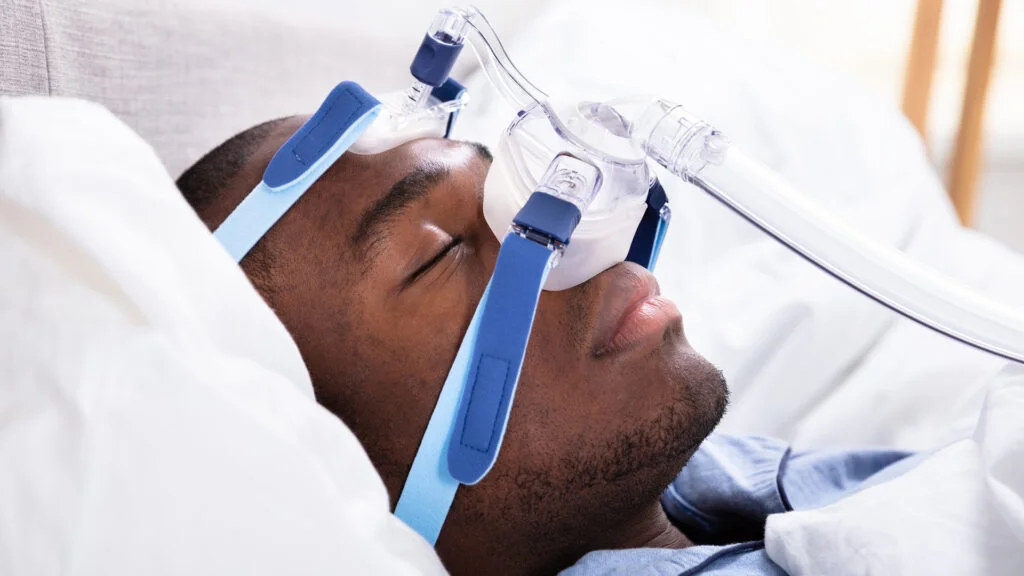
In a continued effort to uncover the wide number of disparities in the healthcare system, including diagnostic testing, researchers recently learned that standard testing for Obstructive Sleep Apnea (OSA) might be underserving Black patients, misrepresenting their results.
During an American Thoracic Society conference, held between May 19 – 24 in Washington D.C., researchers Ali Azarbarzin, assistant professor at Harvard Medical School, along with other researchers from Brigham and Women’s Hospital, released findings that point to potential underestimation in Black participants’ oxygen desaturation compared to white participants. They studied nearly 2,000 patients of varying races and ethnicities who participated in overnight home sleep studies, looking at their oxygen levels after each breathing pause, a common metric used in diagnosing OSA.
The study included oximeters, which may have varying results based on skin pigmentation, Azarbarzin said in the press release. “We did not know whether the same would be true during tests for OSA,” he added, hypothesizing that it would be. The researchers were right, and found that Black participants had a smaller decrease in oxygen saturation (blood oxygen level) for each breathing pause. They adjusted for potential other variables that might have impacted the results, such as BMI, smoking habits, age, and sex.
This is one of many studies that show deep inconsistencies in diagnosis and care for Black versus white populations, further contributing to the increased risk Black people have for OSA. Black Americans aren’t tested and treated as thoroughly or frequently as white Americans, and experts point to implicit bias, cultural beliefs that affect healthcare access, and socioeconomic status, to name just a few challenges. Those sleep differences can be to blame for around half of all discrepancies in health outcomes between white and Black people as well, studies show.
Azarbarzin and his team are concerned that this underestimation the research revealed might lead to “measurement problems” along with an “underestimation of the severity of OSA in Black individuals.” But, he says in the press release, he’s still unclear on whether the oxygen drop underestimation should lead to significant changes in how providers diagnose and handle OSA in Black patients, or others with dark skin, yet.
But, the important research points to a need for “rigorously” testing oximeter accuracy across a diverse population, he explains, and also considering if other factors are contributing to those differences in numbers. All eyes will remain on how researchers next explore if testing needs to be altered for various demographics, especially as technology evolves, such as AI-related tools that can detect race-ethnicity traits too.

Types of Insomnia — Causes and Treatments

Everything You Need to Know About CPAP Devices
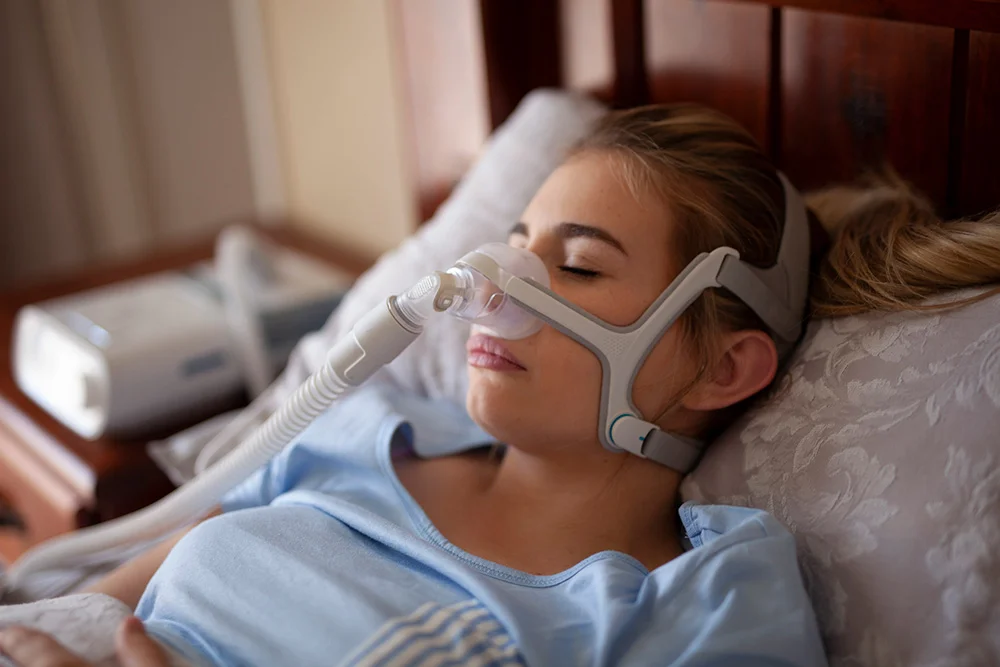
If We Want People to Use Their CPAP Machines, They Need to Be Easier to Use: Opinion

Is Your CPAP Machine Causing You to Gain Weight?
Sources
A. Azarbarzin, G. P. Labarca, T. Sofer, D. Vena, L. Messineo, D. Wellman, D. P. White, S. A. Sands, S. S. Redline; Medicine, Harvard Medical School, Boston, MA, United States, Sleep Medicine, Brigham and Women’s Hospital, Boston, MA, United States, Sleep Medicine, Brigham and Women”s Hospital, Boston, MA, United States, Research, Brigham and Women”s Hospital, Boston, MA, United States, Sleep and circadian disorders, Harvard Medical School, Boston, MA, United States, Brigham and Women’s Hospital, Denver, CO, United States, Division of Sleep and Circadian Disorders, Brigham and Women”s Hospital / Harvard Medical School, Boston, MA, United States, Dept of Med & Div of Sleep Med, Brigham and Women”s Hospital, Boston, MA, United States.
Michael W. Sjoding, M.D., Robert P. Dickson, M.D., Theodore J. Iwashyna, M.D., Ph.D., Steven E. Gay, M.D., Thomas S. Valley, M.D. University of Michigan Medical School, Ann Arbor, MI. “Racial Bias in Pulse Oximetry Measurement,” The New England Journal of Medicine. December 17, 2020.

























