Mental health professional, Joshua McKivigan, was diagnosed with sleep apnea (OSA) about a year ago. He didn’t receive his CPAP machine until months later, and when the Pittsburgh-based dad did get it, he says it “didn’t go well at all.”
“The nasal mask was not a fit for me as I often felt like I couldn’t breathe. After giving it a try for a little over a month and talking with a respiratory therapist, I was given the full mask to try,” he says, though he does feel more alert and has better quality of sleep when he wears it.
He struggled to meet the “4-hour mark,” an indicator that you are using the machine effectively and long enough, as standard insurance companies use to determine if they should keep covering the device for that patient. Most frustrating of all, he struggles with red marks and bruising the machine leaves on his face after use.
“It probably sounds super lazy but I miss just being able to lay my head on a pillow without having to think about putting a mask on,” he says. “Also, my mask does leave red marks on me which aren’t exactly super professional looking when you show up to work looking like you were in a bar fight. I have read into and asked for help with mask fit but this has remained a struggle for me.”
Though he’s improved at meeting the 4-hour mark, he says the only reason he does it is to prevent disrupting sleep for his children and wife with his snoring when he’s not using the machine. “If I was living alone, to be honest, I wouldn’t use it at all because it’s not that comfortable…” he says. “Using the CPAP machine is me trying to help the people I live with get sleep instead of listening to me snore all night.”
McKivigan is far from alone in struggling with one of the most prescribed treatments for sleep apnea. Some patients, especially at 2 a.m. in frustration, might take off the machine wondering how much it will really help anyway. But it’s a risky disease not to treat — University of Chicago Medicine notes that OSA is linked to serious health conditions, such as stroke, diabetes, and hypertension, and increases the risk of car accidents and workplace injury from being overtired in the daytime.
Here’s what experts and innovators in the CPAP compliance space want more people to know, for better sleep and better health.

CPAP Machine Compliance, Defined
The last thing you want to have to worry about when you finally hit your pillow at night is “adherence” or “compliance,” but for those with OSA, that’s an everyday reality. Dr. Carleara Weiss, Ph.D., MS, RN and Aeroflow Sleep’s Sleep Science Advisor, says patients have to have at least 4 hours each night on the machine, for 70 percent of the nights, to benefit from it. This standard is through the American Academy of Sleep Medicine, she says, and also considered by Medicare and insurance. Medicare will then check compliance over 30 consecutive days, anytime during the first three months of initial usage.
From there, the doctor will evaluate how many hours per night the equipment was used, and if your Apnea-Hypopnea Index (AHI) changes, also looking for leaking rate and signs of improved sleep, she adds. This process determines not only whether insurance will continue to cover the machine, but is also seen as helpful to health improvements for OSA with CPAP.
Sleep medicine specialist Dr. Jose Colon in Fort Myers, Fla. adds that the 90-day rule can become problematic as he’s had patients love it the first night, and others who have taken a full year to get used to it.
“Sometimes insurance will give you the option of either returning the machine, or if you don’t want to return it, you need to pay for it yourself. Or sometimes they require a repeat sleep study to qualify,” he says, pointing out the irony here, because the sleep study costs more (for insurers) than the sleep study itself. Doctors are also able to sometimes document severe disruptions in the patients’ ability to use it in the first three months, such as a hurricane or hospitalization disrupting best intentions.
New Research on CPAP Machine Compliance and the “4-Hour Rule”
Though the “4-hour rule” has long been the norm determining “success” with the CPAP, Colon calls the number “arbitrary.” “No one can tell us where those numbers came from. It’s something along the lines of just the way we’ve always done it,” he says. He recommends patients wear the mask the entire time they are sleeping, not just four hours. “As a physician, I do recommend that people breathe when they’re asleep — all of the night, not only four hours, and every night, not just 70 percent.”
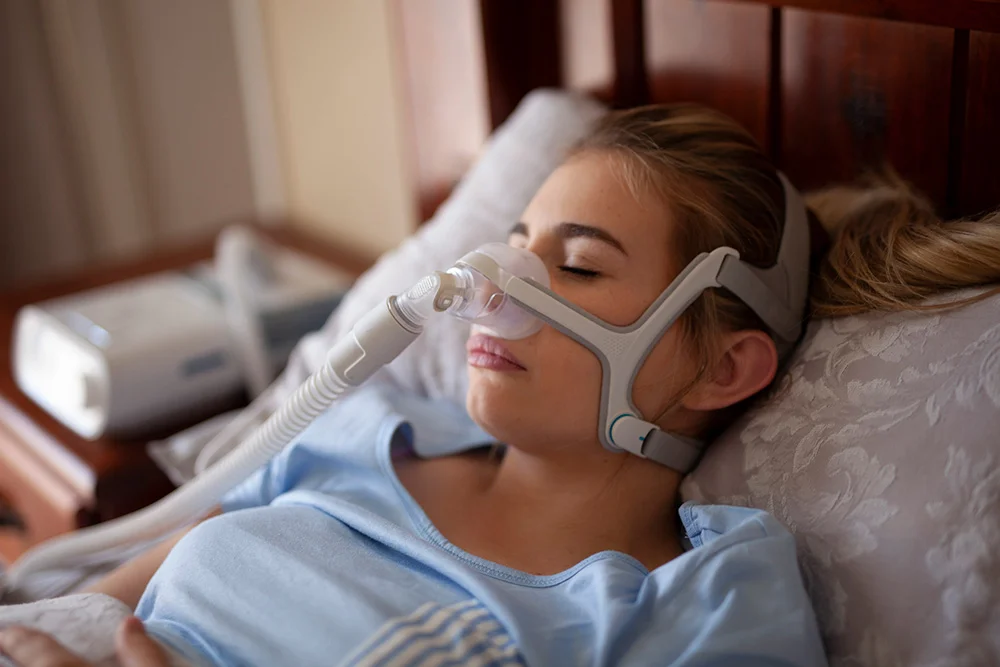
Yet, only around half of patients using the CPAP hit this adherence goal. Typical complaints include feeling claustrophobic, the mask being uncomfortable, and it being difficult to move around. So, scientists out of University of Chicago Medicine and Northwestern recently released a December 2022 study arguing that the four hour definition is inadequate. They are working on a new mobile health technology to address patients’ specific needs and pain points.
In a Dec. 5 2022 press release from U. Chicago Med, researcher Dr. Esra Tasali says, “Sleep apnea can be effectively treated only when CPAP is used during the entire time in bed sleeping.” Their tool provides a new differentiated metric than the generic four hours — a percentage of time a user wears their CPAP, relative to their objectively assessed time spent sleeping. If someone is only using CPAP for four of their eight hour sleep, they are getting the equivalent of a half dose of treatment. Tasali’s team developed the wearable tracker to help patients have a more “meaningful metric.” It also tracks additional metrics like diet, activity, weight goals, and more, to take a comprehensive approach towards improving OSA.
Northwestern research team leader Bonnie Spring explains in the release that these issues often happen together, so the tool is helping people change multiple risk behaviors at the same time. Tasali adds it’s another tool for providers as well to get a more accurate picture of the patient’s progress through monitoring. Next, Tasali wants to study the impact of percent CPAP adherence on health outcomes such as blood pressure and sugar levels.
Barriers to CPAP Machine Compliance, and Alternatives on the Horizon
Changing the metrics might not have much of an impact if you are ripping off the machine in your sleep, however, as one of the major barriers to CPAP compliance is that it can be plain uncomfortable to wear.
“Patients commonly report feeling claustrophobic, nasal irritation or congestion, eye irritation, and air leak. The recommendation to overcome these issues start with appropriate mask fitting and evaluating the air pressure,” Weiss says. “A comfortable, well-adjusted mask minimizes claustrophobia, air leak, and overall discomfort. In addition, having accurate air pressure minimizes nasal congestion and nasal and oral irritation.”
OSA sufferers have sometimes turned to their own solutions, such as Pad-A-Cheek inventor Karen Moore, who woke up after trying her new machine with marks on her cheeks. “I thought, ‘Hm, I don’t have to have that. I’m not a vain person but I don’t need that.’ So I went to my fabric stash and grabbed some pads and flipped them on my straps, and I didn’t have marks on my face the next day,” she says. She realized others in her small town might have the same issue, and sold five more pairs quickly by walking around learning about others’ issues with their CPAP machines as well. Her business expanded substantially, to what is now a well-known brand with medical suppliers, as she has more than 70 products solving issues with machine comfort and use. She still prides herself on quality customer service, helping each client who struggles and sometimes making one of a kind solutions to help them sleep better.
Beyond comfort and face marks, Colon adds that it can be anxiety-related, and others have a dermatitis skin reaction. He makes the analogy that you have dog vs. cat people, iPhone vs. Android people, and similarly, those who have life-changing impacts from CPAP and others who don’t tolerate it. He says others need to have another mechanism of treatment, such as a mandibular device that works more like a retainer.
He says surgeons are now being trained, very recently, on a “great treatment” that can completely treat sleep apnea for some, in which an FDA-approved device called Inspire is implanted into the patient in a same-day procedure. “If it reduces the severity of the sleep apnea 100 percent of the night that you have it on, that’s better than having a 50 percent of the night treatment for sleep apnea,” he says. But, it’s only for certain patients, he adds, such as those without “too high” of a BMI or weight, and OSA severity that isn’t exceptionally high or low. “It’s a sweet spot in the middle.”
In the meantime, reducing barriers to effective CPAP use can mean going in for another fitting, Colon says, as an ill-fitting mask can be the culprit. “There are cloth masks, and when it comes to fittings there are both full face masks and nasal masks,” he says. Nasal masks give more effective treatment, he says, but some need full face masks if they sleep with their mouth wide open. In addition, some medications can be paired with CPAP machines, such as sleep aids, though he says it can be a “slippery slope” to becoming dependent on medication, such as Ambien. One patient, he said, became addicted to the medicine but still didn’t see improvement with CPAP adherence.
Colon recommends a go-to tip that has helped some patients, which is to wear the machine a bit before trying to fall asleep to become more accustomed to it. “We found the more time they have it on while they’re awake, the more acclimated that they become, the more used to it to have it on their face they become, and they stop realizing that it’s on at night and then taking it off.”
Innovations Hoping to Make CPAP Use Easier for Patients
Some brands have made it their mission to solve problems related to CPAP adherence, from those pesky and painful red marks leading to too many questions at work the next day, to leaking from the machine decreasing efficacy. Here are a few making waves in the CPAP compliance industry.
Contour: CPAPPillow2.0
- Keeps CPAP mask in place and the patient comfortable
- Founder Scott Davis says the products help reduce positioning variables that reduce adherence. They also accommodate the CPAP masks and reduce bumping, slipping and resulting leaks. The tether is used to hold the hose and reduce hose drop.
Pad A Cheek: Strap Pad Original Cotton
- Make headgear more comfortable and prevent strap marks on the face
- Provides multiple types of padding, inspired by one the founder’s OSA journey and her sewing savviness, which she uses to make custom products to solve OSA related issues.
NozeSeal: NozeSeal 30-day supply
- Improves CPAP efficacy and comfort, sometimes eliminating the need for headgear
- Reduces leads, and testimonials note their machine stays securely in position
Pur-Sleep: Basic Starter Pack – CPAP Desensitization
- Helps patients get adjusted to CPAP machines. Features aromatherapy, eliminating the “new car smell” of the CPAP
- Uses desensitization processes through olfactory sensors, helping the mind calm down, and refocusing the mind on the smell, not the machine.
Silent Night: CPAP Mask Liner
- Reduces air leaks and improves comfort
- Antibacterial fabric prevents odor-causing bacteria, helping the mask stay cleaner and claiming to reduce cleaning time.
Before trying any of these add-ons, Sleepopolis advises that you speak to your doctor.

Everything You Need to Know About CPAP Devices

A Nasal Spray Sleep Apnea Treatment Shows Promise in New Study

I Had Sleep Apnea For Almost 30 Years: The Inspire Implant Has Been Life-Changing


























