
With an estimated 25 million people suffering from it, obstructive sleep apnea (OSA) is considered the most common sleep-related breathing disorder. (1) (2) Hallmarks of the disorder include loud snoring and pauses in breathing (apneas). Beyond the annoyance of the cacophony, OSA can go far beyond costing you and your partner a good night’s sleep. Short-term symptoms of obstructive sleep apnea include daytime sleepiness, fragmented sleep, irritability, and, of course, the aforementioned snoring and noticeable pauses in breathing. Long-term issues associated with sleep apnea include more complex health issues like high blood pressure, diabetes, stroke, and heart attack.
Obstructive sleep apnea is the most common form of sleep apnea, and CPAP devices are considered the gold standard for treatment. And while CPAP devices can do some pretty heavy lifting to help OSA sufferers find relief, compliance will always be its Achilles heel. (3) Historically, CPAP adherence stalled somewhere between 30 and 60 percent. (4) A more recent study, however, shows compliance rates as low as 25 percent at 12 months post-diagnosis. (4)
Carleara Weiss, Ph.D., MSH, RN, and Sleep Science Advisor for Aeroflow Sleep, says, “Low compliance usually derives from difficulty adjusting to the air pressure, or the mask. Compliance is usually reduced when these two items are not in tune with patient tolerance.” While Weiss notes that these things are easy to adjust at the doctor’s office, she tells Sleepopolis that many patients stop using CPAP rather than reaching out for help or returning to the clinic for titration.”
And when OSA patients hit what they perceive as another brick wall, they’ll likely resume the search for alternatives. And there’s no shortage of alternatives. Ahead, we’ve rounded up some of the most popular non-CPAP-device options out there.
Hypoglossal Nerve Stimulation (HNS)
“Hypoglossal nerve stimulation (HNS) is an OSA treatment that uses an implantable device inserted near the collarbone,” says Weiss. “The device sends electrical impulses to the hypoglossal muscle (the muscle that moves your tongue), which prevents it from collapsing and blocking the airways during sleep. When it works, it reduces snoring, gasping for air, and choking during sleep.” The device also comes with a remote that patients use to turn the device on before sleep and off when they wake.
“Hypoglossal nerve stimulation is typically indicated for people who did not benefit from CPAP (after using it according to compliance), says Weiss. “It works best in slim people (BMI less than 35) because surgical recovery is delicate, and it’s not the best choice if the person has multiple co-morbidities.”
As of 2023, the Inspire™ implant was the only hypoglossal nerve stimulator approved by the Food and Drug Administration. Placement requires a 90-minute outpatient procedure, after which patients typically only need over-the-counter pain medication and can resume normal non-strenuous activities within a few days. According to the brand
- 90 percent of bed partners reported only soft snoring or no snoring at all
- 79 percent reported a reduction in sleep apnea events
Oral Appliances
Patients with mild to moderate obstructive sleep apnea or those who haven’t had any success with CPAP treatment may do better with oral appliances. (5) This category includes Mandibular advancement devices (MAD) and MAD splints. (5) Among oral appliances, mandibular advancement devices are the most frequently prescribed. (5)
Weiss explains, “These devices are worn in the mouth and work by pushing the mandibula forward to help keep the airway open during sleep.” She adds that while these devices “can be used for people with mild OSA, they’re also helpful in specific cases where anatomical problems cause OSA. For example, people with small jaws or TMJ.” Weiss also notes that oral appliances act on the mouth and mouth structures, so they may not resolve OSA issues for someone who is overweight, for example. Or if the problem is on the neck rather than the jaw.”
While patients can try self-moldable devices, custom-made titratable devices are recommended.
This type of MAD device typically consists of dynamically connected pieces covering the teeth of the upper and lower jaw, which can be fine-tuned through titration. (5) One study examining the difference between the two found that custom-made devices were more tolerable by patients (boosting compliance) and ultimately yielded a reduction in sleep apnea events by at least 50 percent in 96 percent of patients. (6) Meanwhile, only 64 percent of patients showed the same reduction in events when wearing self-moldable devices. (6)
Now, while oral appliances may sidestep many of the issues associated with CPAP treatment, they do have some shortcomings, including:
- The time and expense for a customization
- Patients must have a minimal amount of healthy teeth for use
Side effects of oral appliances include:
- Discomfort of the temporomandibular joint
- Tooth pain
- Dry mouth or hypersalivation
- Bite changes over the long term
Continuous Negative External Pressure (cNEP)
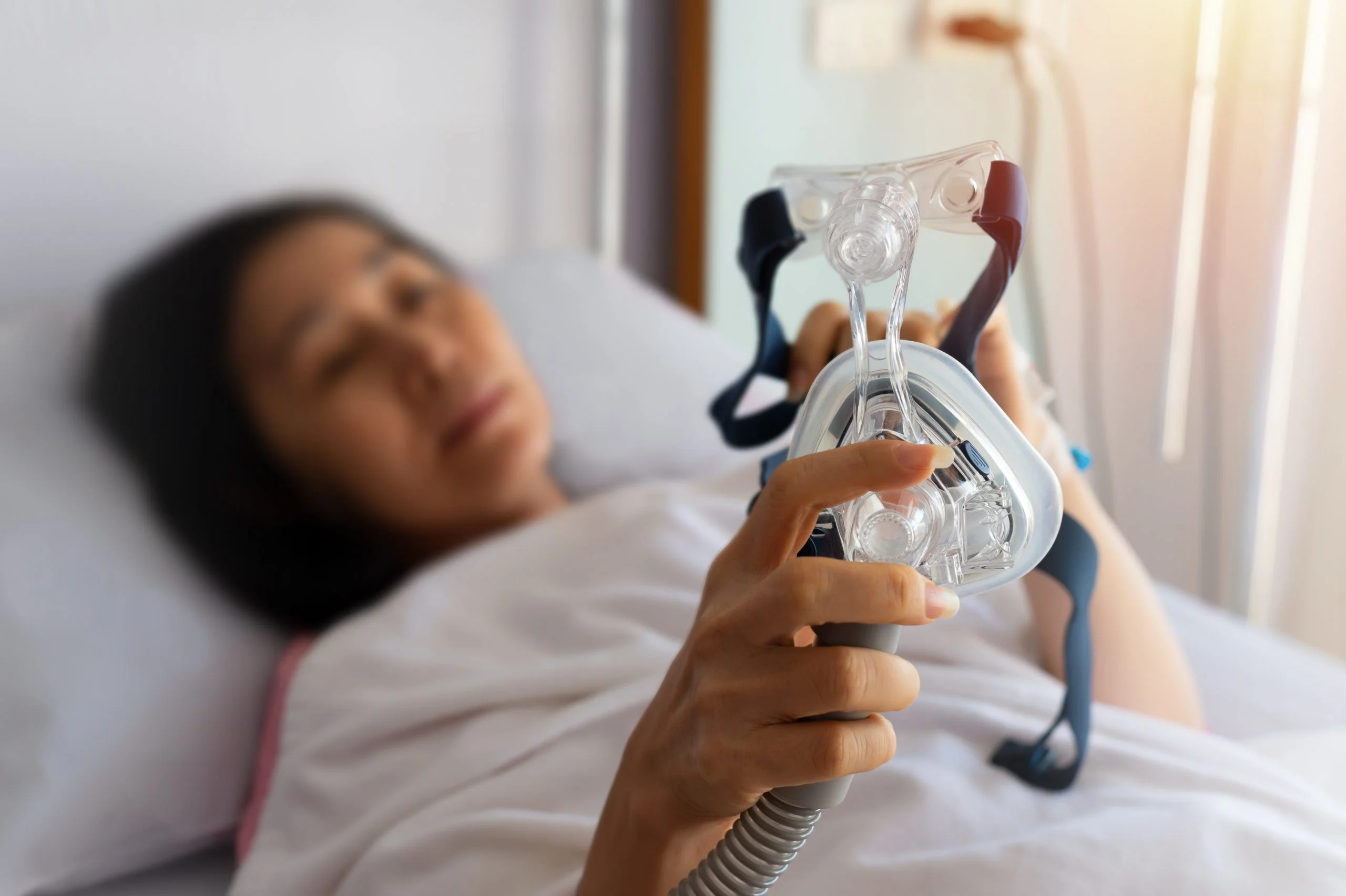
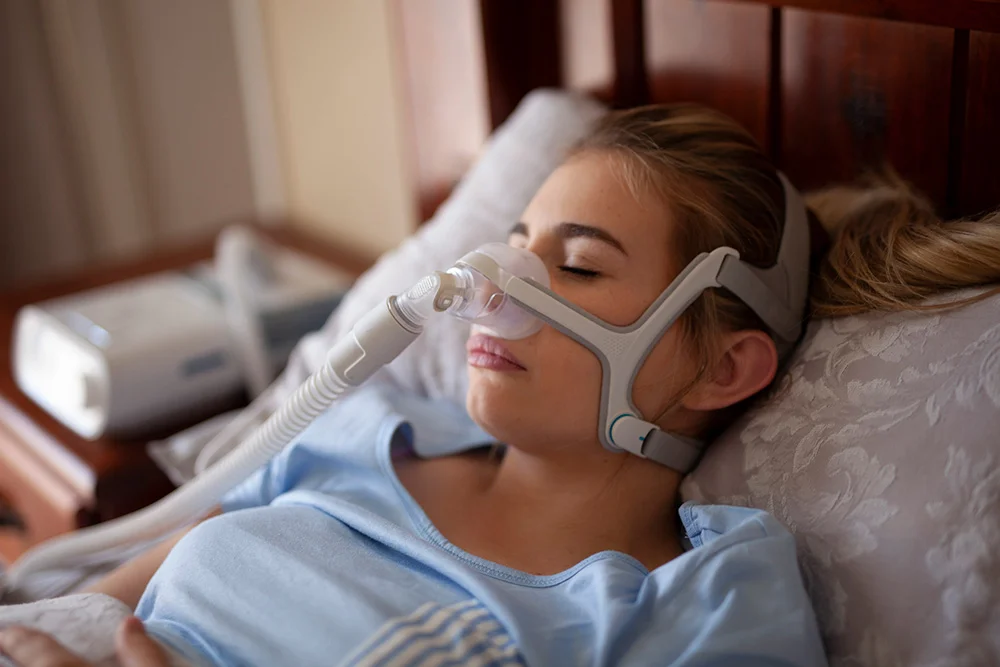
CPAP devices, or continuous positive airway pressure, involve a machine that delivers air through a mask worn during sleep. Air pressure from the device keeps airways open and prevents pauses in breathing. CPAP treatment is considered invasive, as it requires a mask worn over the face all night long to be effective.
Those looking for something less invasive may find it with a Continuous negative external pressure (cNEP) device. (7) This is kind of the “opposite pressure” of a CPAP,” says Weiss. “The device attached outside the neck and “suction it” during sleep to prevent airway collapse.”
cNEP devices consist of a soft silicone collar fitted over the neck. The collar is connected to an adjustable vacuum pump by a flexible tube. The device creates negative pressure that essentially pulls at the throat to prevent airway collapse. (7)
cNEP devices don’t cover the patient’s face or force air into the airways, and heavy hoses aren’t part of the deal either. As a result, patients may find it easier to acclimate to cNEP devices and stick to the treatment over the long term.
In terms of efficacy, a pilot study from 2017 suggested that cNEP treatment may be a viable treatment for OSA — 60 percent of participants dropped down to fewer than 5 AHI events, while 27 percent had at least a partial response. (7)
Other Non-CPAP Devices
In addition to implantable and oral devices, other non-CPAP devices include oral pressure and tongue training devices.
Oral pressure therapy (OPT)
While the research we found is a bit dated, oral pressure therapy may be a viable option for some OSA sufferers. The treatment involves a mouthpiece that essentially creates a vacuum in the oral cavity. It draws the soft palate forward to keep airways open during sleep and allow nasal breathing. Oral pressure therapy is notably quieter than CPAP, and research (though dated) shows that success rates vary between 25 and 37 percent. (8)
Tongue-retaining devices
A tongue-retaining device is a plastic splint that holds the tongue forward to help alleviate snoring or sleep apnea. A healthcare provider or dentist must properly fit the device, and it’s typically recommended for those who can’t tolerate CPAP treatment or those with airway obstructions due to a large tongue. Research shows that tongue-retaining devices can reduce apnea events by 53 percent, but common issues include: (9) (10)
- Device slippage or displacement during the night
- Hypersalivation or drooling
- Dry mouth
- General discomfort/strange sensation on the tongue
What to Consider When Choosing a Treatment for OSA
Considering the amount and severity of adverse health outcomes associated with obstructive sleep apnea, it’s probably best not to let it go untreated. But, like all ailments and disorders, there is no one-size-fits-all treatment. While CPAP works for plenty of people, it may not work for you. After diagnosis, there’s certainly no harm in taking the time to arm yourself with information and weigh your options.
While doing so, Weiss says patients should first take their co-morbidities into account. “As much as having an alternative to a CPAP mask sounds great, not everyone qualifies for those,’ she says. “Furthermore, the CPAP is the gold standard because it can be used by almost everyone, which is not the case with other alternatives.” Additionally, Weiss says patients should “Follow the clinician’s instructions. There is a lot of information on social media, etc., and nothing replaces clinical evaluation.”
A Revolutionary Device For Treating Sleep Apnea Is Headed For IPO

Everything You Need to Know About CPAP Devices
FDA Issues New Recall Alert For ResMed CPAP Devices: Here’s What to Know

10 Sleep Trends for 2024: Separating Fads from Science
Sources
1. Kingshott, R. (2017, November 7). Rising prevalence of sleep apnea in U.S. threatens Public Health. American Academy of Sleep Medicine – Association for Sleep Clinicians and Researchers. https://aasm.org/rising-prevalence-of-sleep-apnea-in-u-s-threatens-public-health/
2. Cumpston E, Chen P. Sleep Apnea Syndrome. [Updated 2023 Sep 4]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK564431/
3. Batool-Anwar S, Goodwin JL, Kushida CA, et al. Impact of continuous positive airway pressure (CPAP) on quality of life in patients with obstructive sleep apnea (OSA). J Sleep Res. 2016;25(6):731-738. doi:10.1111/jsr.12430
4. Qiao, M., Xie, Y., Wolff, A. et al. Long term adherence to continuous positive Airway pressure in mild obstructive sleep apnea. BMC Pulm Med 23, 320 (2023). https://doi.org/10.1186/s12890-023-02612-3
5. Verbraecken J, Dieltjens M, Op de Beeck S, et al. Non-CPAP therapy for obstructive sleep apnoea. Breathe (Sheff). 2022;18(3):220164. doi:10.1183/20734735.0164-2022
6. Francis, C.E., Quinnell, T. Mandibular Advancement Devices for OSA: An Alternative to CPAP?. Pulm Ther 7, 25–36 (2021). https://doi.org/10.1007/s41030-020-00137-2
7. Kram JA, Woidtke RV, Klein KB, Rose RM. Evaluation of Continuous Negative External Pressure (cNEP) for the Treatment of Obstructive Sleep Apnea: A Pilot Study. J Clin Sleep Med. 2017;13(8):1009-1012. Published 2017 Aug 15. doi:10.5664/jcsm.6710
8. Nigam G, Pathak C, Riaz M. Effectiveness of oral pressure therapy in obstructive sleep apnea: a systematic analysis. Sleep Breath. 2016;20(2):663-671. doi:10.1007/s11325-015-1270-3
9. Edward T. Chang, Camacho, M., Barthlen, G. M., Adachi, S., Farrow, S. J., Ihara, K., Shinagawa, H., Chen, H., Ono, T., Cartwright, R., Jun, J. C., Levy, P., Wolfe, R. M., Bratton, D. J., … Caldarelli, D. D. (2017, January 18). Tongue retaining devices for obstructive sleep apnea: A systematic review and meta-analysis. American Journal of Otolaryngology. https://www.sciencedirect.com/science/article/abs/pii/S0196070916304197
10. Waled M. Alshhrani , BDS, MS, PhD(c) ; Mona M. Hamoda , BDS, MSc, MHSc, PhD(c) ; Kentaro Okuno , PhD ; Yuuya Kohzuka , PhD ; John A. Fleetham , MD ; Najib T. Ayas , MD ; Robert Comey , MD ; Fernanda R. Almeida , DDS, MSc, PhD. The efficacy of a titrated tongue-stabilizing device on obstructive sleep apnea: a quasi-experimental study. Journal of Clinical Sleep Medicine. 2021; 17 (8 doi.org/10.5664/jcsm.9260
Weiss, Carleara. Author interview. February 21, 2024.

























