
A relatively new treatment for obstructive sleep apnea (OSA) is making it easier to get a restful night of sleep. Sleep apnea is a potentially serious sleep disorder in which breathing repeatedly stops during the night, resulting in night wakings and low oxygen levels. There are multiple types of sleep apnea, but obstructive sleep apnea, in which the throat muscles relax and block the airway, is the most common. Untreated, obstructive sleep apnea can lead to daytime tiredness, memory issues, and increased risk of heart disease.
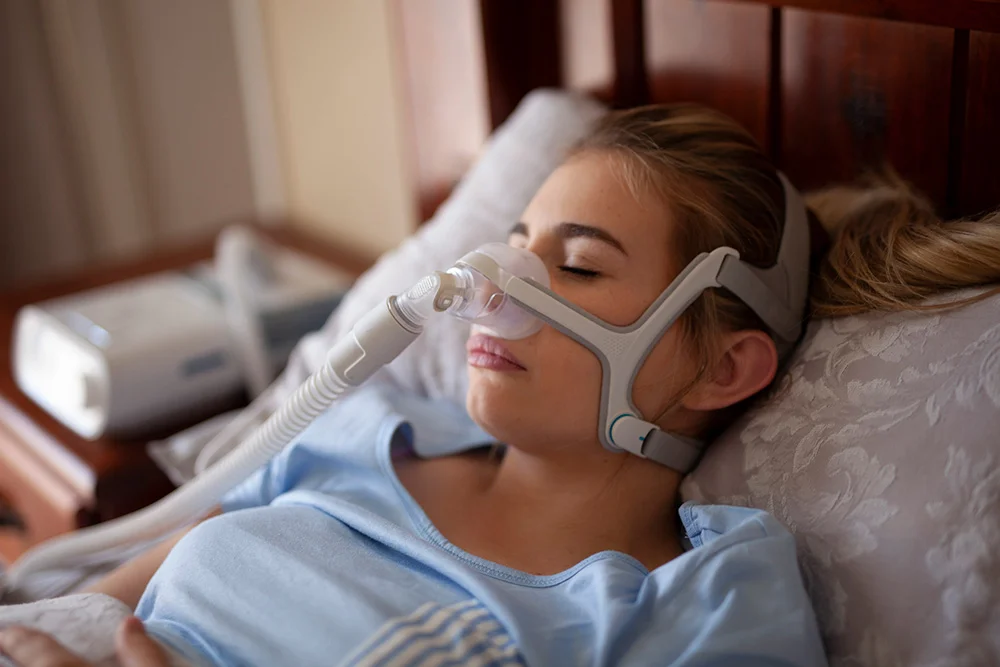
A recent study estimates that over a quarter of Americans aged 30 – 70 years old are affected by OSA and historically, the first line of treatment was a continuous positive airway pressure (CPAP) machine. This device is easily accessible, but it is loud, often uncomfortable, and has a poor usage rate. Due to low compliance with the machine, doctors and patients are increasingly looking to non-CPAP devices for relief. Dr. Robert Philip Lindeman, a retired pediatric pulmonologist and sleep specialist, tells Sleepopolis that “There are several reviews in the literature that found upper airway stimulation to be effective in treating OSA, particularly in patients who cannot tolerate CPAP.”
Hypoglossal Nerve Stimulation (HNS) Therapy
In 2014, a device called Inspire was approved by the FDA. Unlike a CPAP machine, the implant is undetectable by bed partners, is comfortable, and never requires cleaning. The implant provides Hypoglossal Nerve Stimulation (HNS), also sometimes called Upper Airway Stimulation (UAS) to keep the airways open and prevent lapses in breathing. The device is implanted during a minimally invasive outpatient procedure in which two incisions are made; one under the chin where a small nerve cuff is placed, and one in the upper chest to implant the device. After the patient recovers, they can go back to the doctor’s office to work with the provider to set up the device and determine the correct level of stimulation. Then, before bed, the patient uses a remote control to turn on the device. It then automatically shuts off after a certain amount of time (based on the individual’s average night of sleep).
Complications from hypoglossal nerve stimulation are low compared to the CPAP machine and compliance has proven to be much higher. Research shows that half of all CPAP machine users discontinue use within 12 months while compliance with HNS is estimated to be 86 percent at 12 months.
Who It’s For and Why
While hypoglossal nerve stimulation (or upper air stimulation) is a novel treatment with a lot of potential, it’s not for everyone. In general, CPAP or BIPAP machines are still the first line of treatment. But the implants are a good alternative for people who cannot tolerate CPAP or BIPAP machines. Depending on the health care provider, there may be other requirements and restrictions.
In general, eligible patients should be age 18 or older, have a BMI of less than 35, and exhibit moderate to severe obstructive sleep apnea. While the treatment is promising, Dr. Sony Sherpa, a physician and practitioner of holistic medicine, says there are many factors to consider.
“The primary advantage of UAS treatment is that it allows patients unobstructed breathing without having to rely on cumbersome or uncomfortable devices,” Dr. Sherpa says. “However, this therapy requires minor surgery to implant the device, and thus carries associated risks, such as infection and failure due to poor tissue tolerance.” She cautions, “Other potential side effects include dental injury, pain in the throat area, and discomfort at the site of implant. Moreover, there may be financial considerations, as insurance coverage for this type of therapy is not universal.”
FDA Approval
Currently, the Inspire device is the only FDA-approved implant for obstructive sleep apnea although similar products are in development. For individuals with central sleep apnea (CSA), the remedē device is an implant that works similarly. In addition to breathing masks and implants, individuals may also be able to treat sleep apnea through mandibular advancement devices, tongue retaining devices, changing sleep positions, or losing weight. The important thing is finding something that a patient finds comfortable and will use regularly since reducing night wakings can go a long way in improving sleep quality and maintaining overall health.

I Had Sleep Apnea For Almost 30 Years: The Inspire Implant Has Been Life-Changing
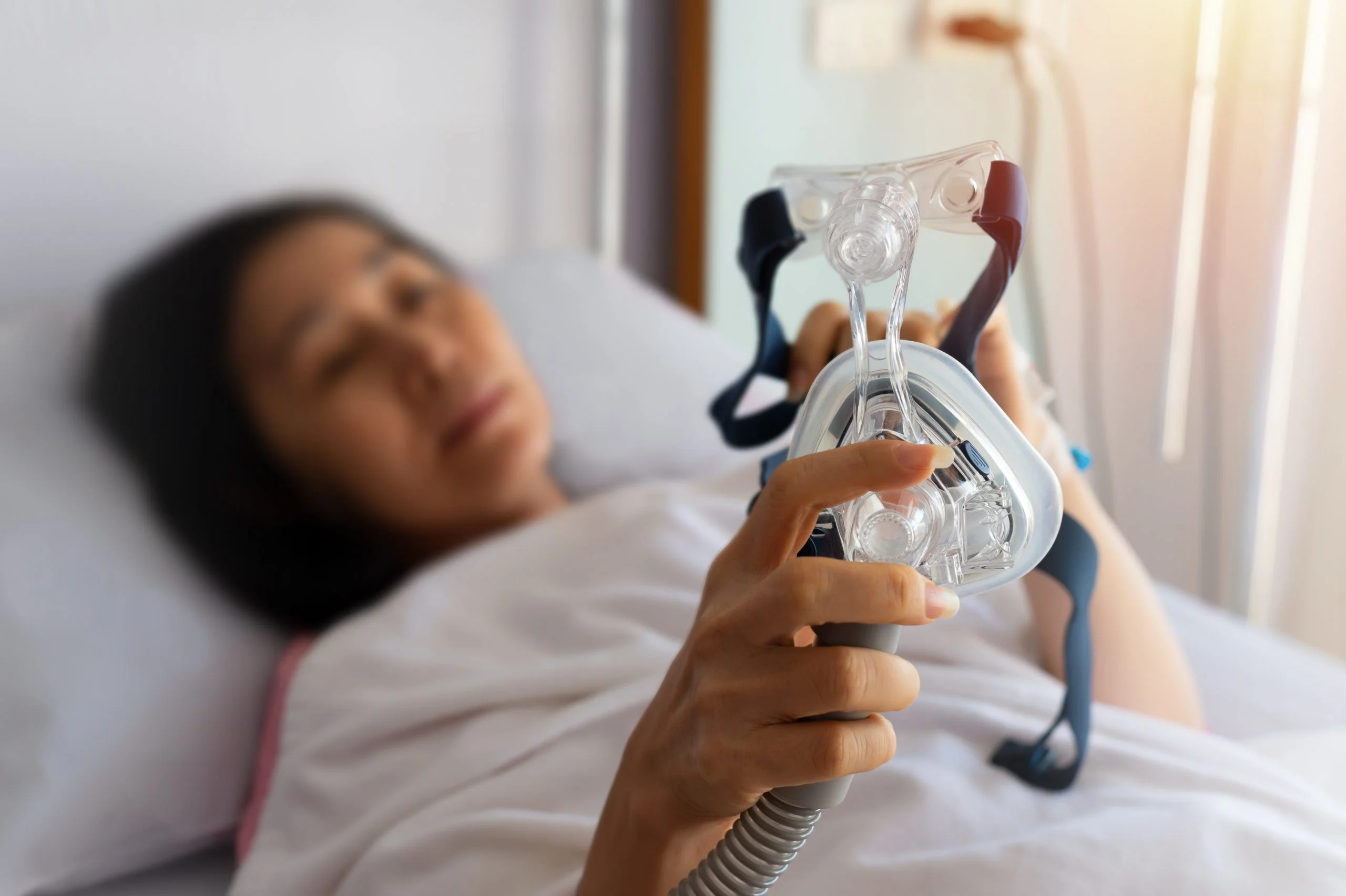
If We Want People to Use Their CPAP Machines, They Need to Be Easier to Use: Opinion

FDA Assigns its Most Serious Designation in New Philips CPAP Machine Recall: What to Know
New Sleep Apnea Research Promises Hope Beyond CPAP Machines in the Form of a “Magic Pill”
Sources
Santilli M, Manciocchi E, D’Addazio G, Di Maria E, D’Attilio M, Femminella B, Sinjari B. Prevalence of Obstructive Sleep Apnea Syndrome: A Single-Center Retrospective Study. Int J Environ Res Public Health. 2021 Sep 29;18(19):10277. doi: 10.3390/ijerph181910277. PMID: 34639577; PMCID: PMC8508429.
Otto D. Schoch, Florent Baty, Jolanda Niedermann, Jochen J. Rüdiger, Martin H. Brutsche; Baseline Predictors of Adherence to Positive Airway Pressure Therapy for Sleep Apnea: A 10-Year Single-Center Observational Cohort Study. Respiration 1 February 2014; 87 (2): 121–128. https://doi.org/10.1159/000354186
Lindeman, Robert Philip. Author interview. June 2024.
Wray CM, Thaler ER. Hypoglossal nerve stimulation for obstructive sleep apnea: A review of the literature. World J Otorhinolaryngol Head Neck Surg. 2016 Dec 22;2(4):230-233. doi: 10.1016/j.wjorl.2016.11.005. PMID: 29204571; PMCID: PMC5698546.
Sherpa, Sony. Author interview. June 2024.


























